Teeth for Life
At birth people usually have 20 primary (baby) teeth, which often erupt through the gums as early as six months of age.
These teeth are then shed at various times throughout childhood. By age 21, all 32 of the permanent teeth have usually erupted.
Learn more
getting to know your teeth is fun! Learn all about your teeth with our fun, interactive and educational diagrams:
- Know Your Teeth
- Anatomy of a Tooth
Regular Checkups
Don't brush off regular checkups to the dentist! Regular dental checkups are essential to maintaining good oral health. WE encourage regular checkups at least every six months. Seeing the dentist twice a year is recommended because your dentist can:
- Check for problems that you might not see or feel
- find early signs of decay
- treat oral health problems early, while they are still manageable
Regular checkups include a thorough cleaning, polishing, and an oral exam by the doctor. During the oral exam, the doctor checks the health of your mouth, teeth, gums, cheeks, and tongue. At each visit, the doctor also checks old fillings and restorations because constant pressure from chewing, grinding, or clenching can cause them to wear away, chip, or crack.
Your First visit
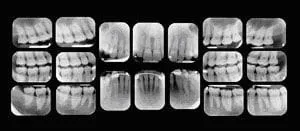
Your first visit to the doctor typically includes an x-ray that allows the doctor to view the structure of the jaw, the position of any teeth that have not yet erupted, malformed roots, and tooth decay.
The initial visit also involves getting your medical history. When you share your medical history with the doctor, be sure to provide complete, up-to-date information on your health. Inform your dentist if you have experienced recent hospitalization or surgery, or if you have recently been ill. Also tell the doctor the names, doses and frequency of any medication you are taking whether prescription or over-the-counter products -- and the name of your physician. Inform the doctor of any changes in your health or medications. It is also important to bring up any fears you may have about dental treatment.
The information collected in your first visit will help the doctor select the safest and most effective method of treatment for you.
Improve Your Smile
With recent advances in dental care, you can have an attractive smile. You don't have to settle for stained, unsightly teeth. Rather, you have choices that can help you smile with confidence.
A subtle change in your smile can make a big difference in the way you look and feel about yourself. Talk to the doctor about the options most suitable for you, what your expectations are and the dental fees involved.
Toothed Whitening Treatments
Everybody loves a bright white smile, and there are a variety of products and procedures available to help you improve the look of yours.
Many people are satisfied with the sparkle they get from brushing twice daily with a fluoride-contain toothpaste, cleaning between their teeth once a day, and the regular cleaning at the dentist's office. However, if you decide you would like to go beyond this to make your smile look brighter, you should investigate all of your options.
You can whiten your smile in one appointment with the doctor or you can use an at-home bleaching system) (store-bought or from your dental office) or whitening toothpaste.
What should you ask the doctor?
You may want to start by speaking with the doctor. He or she can tell you whether whitening procedures would be effective for you. Whiteners may not correct all types of discoloration. For example, Yellowish-hued teeth will probably bleach well, brownish-colored teeth may bleach less well, and grayish-hued teeth may not bleach well at all. Likewise, bleaching may not enhance your smile if you have had tooth-colored fillings placed in your front teeth. The whitener will not affect the color of these materials, and they will stand out in your newly whitened smile. In these cases, you may want to investigate other options, like porcelain veneers.
What is in-office bleaching?
If you are candidate for bleaching, the doctor may suggest a procedure that can be done in our office. This procedure is called chair-side bleaching and may require more than one office visit. Each visit may take from 60 to 90 minutes.
During chair-side bleaching, the dentist will apply either a protective gel to your gums or a rubber shield to protect the oral soft tissues. A bleaching agent is then applied to the teeth, and a special light may be used to enhance the action of the agent.
A number of in-office bleaching agents have the ADA Seal of Acceptance, your assurance that they have met ADA standards of safety and effectiveness.
What are at=home procedures and products
There are several types of products available for use at home, which can either be dispenses by the doctor or purchased over the counter.
Bleaching solutions
These products contain peroxide(s), which actually bleach the tooth enamel. These products typically rely on ceramide peroxide as the bleaching agent; ceramide peroxide comes in several different concentrations (10%, 16%, and 22%).
Peroxide-contain whiteners typically come in a gel and are placed in a mouth guard. Usage regimens vary. Some products are used twice a day for 2 weeks, and others are intended for overnight use for 1-2 weeks. If you obtain the bleaching solution from the doctor, he or she can make a custom-fitted mouth guard for you that will fit your teeth precisely. Currently, only dentist dispensed home-use 10% ceramide peroxide tray-applied gels carry the ADA Seal.
You also may want to speak with the doctor should any side effects become bothersome. For example, teeth can become sensitive during the period when you are using the bleaching solution. In most cases, this sensitivity is temporary and should lessen once the treatment is finished. Some people also experience soft-tissue irritation, either from a tray that doesn't fit properly or from solution that may come in contact with the tissues. If you have concerns about such side effects, you should discuss them with the doctor.
Toothpastes
All toothpastes help remove surface stain through the action of mild abrasives. "Whitening" toothpastes in the ADA Seal of Acceptance program have special chemical or polishing agents that provide additional stain-removal effectiveness. Unlike bleaches, these ADA Accepted products do not alter the intrinsic color of teeth.
How should I choose a whitening product?
When selecting a whitener or any dental product, be sure to look for the ADA Seal of Acceptance -- your assurance that they have met ADA standards of safety and effectiveness.
Porcelain Veneers and Porcelain Crowns
There's no reason to put up with gaps in your teeth or with teeth that are stained, badly shaped, or crooked. Today a veneer placed on top of your teeth can correct nature's mistake or the results of an injury and help you have a beautiful smile.
Veneers are thin, custom-made shells crafted of tooth-colored materials designed to cover the front side of teeth. Typically a dental technician makes them in a dental lab, working from a model provided by the doctor.
This is usually an irreversible process because it's necessary to remove a small amount of enamel from your teeth to accommodate the shell.
The doctored may recommend that you avoid some food and beverages that may stain or discolor your veneers such as coffee, tea, or red wine. Sometimes a veneer might chip or fracture, but for many people the results are more than worth it.
Restore Your Smile
A smile can be the most eye-catching feature of a face. With dentistry's many advances, you no longer have to settle for stained, chipped, or misshapen teeth. You have choices that can help you smile with confidence. Talk to the doctor about the options most suitable for you, what your expectations are, and the dental fees involved.
Bridges
If you're missing one or more teeth, you may notice a difference in chewing and speaking. A bridge may be used to replace missing teeth, help maintain the shape of your face, and alleviate the stress in your bite. There are two types of tooth replacement: fixed bridge and implant. A fixed bridge replaces missing teeth with artificial teeth, looks great, and literally bridges the gap where one or more teeth may have been. The restoration can be made from gold, alloys, porcelain, or a combination of these materials and is bonded onto surrounding teeth for support. An implant attaches artificial teeth directly to the jaw under the gum tissue. A small titanium fixture may be used to surgically place the implant in the upper or lower jawbone to replace the root of your missing tooth and provide an anchor for a crown. The success of any bridge or implant depends on its foundation: the other teeth, gums, or bone to which it is attached. So it's very important to keep your remaining teeth, gums, and jaw healthy and strong.
Crowns
A crown covers a tooth and restores it to its normal shape and size. A crown can make your tooth stronger and improve its appearance. It can cover and support a tooth that has a large filling. It can be used to attach a bridge, prevent a weak or brittle tooth from breaking, or restore one that's already broken. A crown is a good way to cover teeth that are discolored, badly shaped, or out of position. Crowns are also used to cover dental implants.
A crown may be made of gold or porcelain. It is made to fit the tooth precisely. It looks somewhat like a thimble and is cemented onto the prepared tooth. If the doctor recommends a crown, it's probably to correct one of these conditions. The doctor's primary aim, like yours, is to help you keep your teeth healthy and your smile bright.
Extractions
There are times when it is necessary to remove a tooth. Sometimes a baby tooth has long or misshapen roots that prevent it from falling out and the tooth must be removed to make way for the permanent tooth to erupt. At other times, a tooth may have so much decay that it puts the surrounding teeth and jaw at risk of decay, so the doctor may recommend removal and replacement with a bridge or implant. Infection, orthodontic correction, or problems with a wisdom tooth can also require removal of a tooth.
When it is determined that a tooth needs to be removed, the dentist may extract the tooth during a regular checkup or the dentist may request another visit for this procedure. While the procedure is typically very quick, it is important to share any concerns or preferences for sedation that you may have.
Fillings
Restoring Your Smile: Dental Filling Choices
Advances in modern dental materials and techniques have provided new ways to create more pleasing, natural-looking smiles. As a result, dentists and patients have several choices when it comes to selecting materials used to repair missing, worn, damaged, or decayed teeth. Traditional dental restoratives include gold, porcelain, and composite. The strength and durability of traditional dental materials continue to make them useful for situations where restored teeth must withstand extreme forces that result from chewing, such as in the back of the mouth. Newer dental restoratives include ceramic and plastic compounds that mimic the appearance of natural teeth. These compounds, often called composite resins, are often used on the front teeth where a natural appearance is important. They can be used on the back teeth as well depending on the location and extent of the tooth decay. Composite resins are usually more costly than the older amalgam fillings.
What's right for me?
Several factors influence the performance, durability, longevity, and expense of dental restorations. These factors include: the components used in the filling material; the amount of tooth structure remaining; where and how the filling is placed; the chewing load that the tooth will have to bear; and the length and number of visits needed to prepare and adjust the restored tooth.
With so many choices, how do you know what's right for you?
The ultimate decision about what to use is best determined by the patient in consultation with the dentist. Before your treatment begins, discuss the options with the doctor. To help you prepare for this discussion it is helpful to understand the two basic types of dental restorations: direct and indirect. Direct restorations are fillings placed immediately into a prepared cavity in a single visit. They include dental amalgam, glass ionomers, resin ionomers, and composite (resin) fillings. The dentist prepares the tooth, places the filling, and adjusts it during one appointment. Indirect restorations generally require two or more visits. They include inlays, onlays, veneers, crowns, and bridges fabricated with gold, base metal alloys, ceramics, or composites. During the first visit, the dentist prepares the tooth and makes an impression of the area to be restored. The dentist then places a temporary covering over the prepared tooth. The impression is sent to a dental laboratory, which creates the dental restoration. At the next appointment, the dentist cements the restoration into the prepared cavity and adjusts it as needed.
Implants
If you have missing teeth, it is crucial to replace them. Without all your teeth, chewing and eating can destabilize your bite and cause you discomfort. Implants are a great way to replace your missing teeth. An implant is composed of two parts that mimic a tooth's root and crown. The implant's root is a titanium steel rod that is placed into the jawbone and acts as a root. Once the rod is in place, a crown is then attached to it to replace the top part of your tooth. You now have an entirely new tooth made of steel and porcelain, and it will look just like your natural tooth.
Root Canal (Endodontic) Treatment
In the past, if you had a tooth with a diseased nerve, you'd probably lose that tooth. Today, with a special dental procedure called root canal treatment, you may save that tooth. Inside each tooth is the pulp and the nerve. The nerve is the vestige of the tissue that originally formed the tooth. Once the tooth has been in the mouth for a time, the functioning of the nerve is no longer necessary.
When a tooth is cracked or has a deep cavity, bacteria can enter the pulp. Germs can cause an infection inside the tooth. Left without treatment, pus builds up at the root tip, in the jawbone, forming a "pus-pocket" called an abscess. An abscess can cause the pulp tissue to die. When the infected pulp is not removed, pain and swelling can result. Certain byproducts of the infection can injure your jawbones and your overall health. Without treatment, your tooth may have to be removed.
Treatment often involves from one to three visits. During treatment, your general dentist or endodontist (a dentist who specializes in problems of the pulp) removes the diseased pulp. Next, the pulp chamber and root canal(s) of the tooth are cleaned and sealed. Often posterior teeth that have endodontic treatment should have a cast crown placed in order to strengthen the remaining structure. Then as long as you to continue to care for your teeth and gums with regular brushing, flossing, and checkups so that the root(s) of the restored tooth are nourished by the surrounding tissues, your restored tooth can last a lifetime.
Most of the time, a root canal is a relatively simple procedure with little or no discomfort involving one to three visits. Best of all, it can save your tooth and your smile!
Preventative Dentistry
Preventative dentistry relies on good oral hygiene and regular dental care, and is important throughout your life, whatever your age. By practicing good oral hygiene at home and visiting the doctor regularly, you will help prevent dental problems and save time and money. In the process, you can save your teeth and gums.
Fighting Plaque
By fighting plaque you can keep your teeth for a lifetime. Today, in fact, older adults are keeping their natural teeth longer because of scientific developments and an emphasis on preventative dentistry.
Good oral hygiene requires an understanding of plaque. Plaque is a sticky, colorless layer of bacteria. When you eat carbohydrates (foods made of sugar or starch) you feed this plaque, which in turn produces acids that attack tooth enamel, cause cavities, and develop a hard substance called calculus (tartar). Uninterrupted, the acid attacks can result in tooth decay and gum disease (also known as periodontal disease). If left untreated, gum disease can cause loss of teeth and bone.
At any age, you can begin the fight with plaque and keep your teeth and gums healthy. It's really quite easy. Simply:
- Brush your teeth twice a day with a soft-bristled toothbrush and fluoride toothpaste to remove food particles and plaque from the tooth surfaces. While you're at it, brush the top surface of your tongue to eliminate bad breath and bacteria buildup.
- Clean between your teeth daily with floss or an interdental cleaner. Decay-causing bacteria can linger between teeth where toothbrush bristles can't reach. Flossing removes plaque and food particles from between the teeth and under the gum line.
- Eat a balanced diet and limit between-meal snacks. If a snack is needed, nutritious foods such as raw vegetables, plain yogurt, cheese, or a piece of fruit should be chosen.
- Schedule regular checkups. Visit the doctor regularly (every six months) for professional cleanings and oral exams.
- Ask the doctor about dental sealants, a protective plastic coating that can be applied to the chewing surfaces of the back teeth where decay often starts.
- Wear mouth protection such as a mouthguard when you play contact sports or extreme sports.
Preventing Tooth Decay
Tooth decay (cavity or caries) can develop on any surface of any tooth. Because cavities grow, they are much easier and less expensive to treat when they are small. A decaying tooth may not hurt, so you may have a cavity and not realize it. The dentist checks for tooth decay at your regular checkups and will periodically use x-rays to check for decay between teeth. The dentist treats tooth decay by cleaning out the cavity and placing a restoration (filling) in the tooth.
By following the strategies listed above, you can prevent tooth decay.
Preventing Gum Disease
Gum disease (also called periodontal disease) is an infection of the tissues that support your teeth. It is a major cause of tooth loss in adults. Because gum disease is usually painless, you may not know you have it. At each regular checkup the dentist will measure the depth of the shallow v-shaped crevice (called a sulcus) between your tooth and gums to identify whether you have gum disease.
Gum disease is caused by plaque, a sticky film of bacteria that constantly forms on the teeth. These bacteria create toxins that can damage the gums.
Periodontal diseases attack just below the gum line in the sulcus, where they cause the attachment of the tooth and its supporting tissues to break down. As the tissues are damaged, the sulcus develops into a pocket; generally, the more severe the disease, the greater the depth of the pocket.
Periodontal diseases are classified according to the severity of the disease. The two major stages are gingivitis and periodontitis.
In the early stage of gum disease, called gingivitis, the gums become red and swollen and bleed easily. At this stage, the disease is still reversible and can usually be eliminated by daily brushing and flossing.
In the more advanced stages of gum disease, called periodontitis, the gums and bone that support the teeth become seriously damaged. The teeth can become loose, fall out, or have to be removed by a dentist.
Some factors increase the risk of developing periodontal disease:
- Tobacco smoking or chewing
- System-wide diseases such as diabetes
- Some types of medication such as steroids, some types of anti-epilepsy drugs, cancer therapy drugs, some calcium channel blockers, and oral contraceptives
- Bridges that no longer fit properly
- Crooked teeth
- Fillings that have become defective
- Pregnancy
If you notice any of the following signs of gum disease, see the doctor immediately:
- Gums that bleed easily
- Red, swollen, tender gums
- Gums that have pulled away from the teeth
- Persistent bad breath or bad taste
- Pus between your teeth and gums
- Permanent teeth that are loose or separating
- Any change in the way your teeth fit together when you bite
- Any change in the fit of partial dentures
It is possible to have periodontal disease and have no warning signs.
That is one reason why regular dental checkups and periodontal examinations are very important. Treatment methods depend on the type of disease and how far the condition has progressed.
Good oral hygiene at home is essential to keep periodontal disease from becoming more serious or recurring. You don't have to lose teeth to periodontal disease. Brush, clean between your teeth, eat a balanced diet, and schedule regular dental visits for a lifetime of healthy smiles.
Normal, healthy gums: Healthy gums and bone anchor teeth firmly in place.
Gingivitis: Gums are red and swollen and bleed easily.
Periodontitis: Unremoved plaque hardens into calculus (tartar). As plaque and calculus continue to build up, the gums begin to recede (pull away) from the teeth, and pockets form between the teeth and gums.
Advanced periodontitis: The gums recede farther, destroying more bone and the periodontal ligament. Teeth — even healthy teeth — may become loose and need to be extracted.
The good news is that you can help prevent gum disease by taking good care of your teeth every day and having regular dental checkups.
How to Brush Your Teeth
You should replace your toothbrush every three or four months — or sooner if the bristles become frayed. A worn toothbrush will not do a good job of cleaning your teeth. Children's toothbrushes often need replacing more frequently than adults' because they can wear out sooner.
People who have difficulty handling dental floss may prefer to use another kind of interdental cleaner. These aids include special brushes, picks, and sticks. If you use interdental cleaners, ask the doctor about how to use them properly to avoid injuring your gums.
Choosing Dental Products
When choosing any dental product, look for the American Dental Association Seal of Acceptance, an important symbol of a dental product's safety and effectiveness. Talk to the doctor about what types of oral care products will be most effective for you. The ADA Seal on a product is your assurance that it has met ADA criteria for safety and effectiveness. Look for the ADA Seal on fluoride toothpaste, toothbrushes, floss, interdental cleaners, oral irrigators, and mouth rinse.
By taking care of your teeth, eating a balanced diet, and visiting the doctor regularly, you can have healthy teeth and an attractive smile throughout your entire life.
Dr. Economos is a Certified Invisalign® Provider
Consider Invisalign to get the beautiful straight teeth you've always wanted — without braces. A complimentary consultation with Dr. Economos can determine if Invisalign is right for you.
What is it?
Invisalign uses a series of invisible, removable, and comfortable aligners that no one can tell you're wearing. So, you can smile more during treatment as well as after. Invisalign is made with 3-D computer imaging technology and has been proven effective. More than 70% of orthodontists in the US and Canada are certified to treat with Invisalign.
Why would I want it?
Not only are the aligners invisible, they are removable, so you can eat and drink what you want while in treatment. Plus, brushing and flossing are no problem. They are also comfortable, with no metal to cause mouth abrasions during treatment. And no metal and wires usually means you spend less time in your doctor's office getting adjustments. Invisalign also allows you to view your own virtual treatment plan when you start so you can see how your straight teeth will look when your treatment is complete.
How does it work?
You wear each set of aligners for about 2 weeks, removing them only to eat, drink, brush, and floss. As you replace each aligner with the next in the series, your teeth will move — little by little, week by week — until they have straightened to the final position Dr. Economos has prescribed. You'll visit Dr. Economos about once every 6 weeks to ensure that your treatment is progressing as planned. Total treatment time averages 9-15 months and the average number of aligners worn during treatment is between 18 and 30, but both will vary from case to case.

